NHS rolls out rapid pembrolizumab injection, projecting over 100,000 staff hours saved yearly
The NHS will replace intravenous pembrolizumab with a one‑minute injectable form, projecting over 100,000 saved staff hours yearly and benefiting about 14,000 patients.
TL;DR
The NHS will replace intravenous pembrolizumab with a one‑minute injectable form, projecting a saving of over 100,000 staff hours each year. About 14,000 patients currently receiving the drug are expected to switch, cutting treatment time from roughly two hours to under two minutes per session.
Context
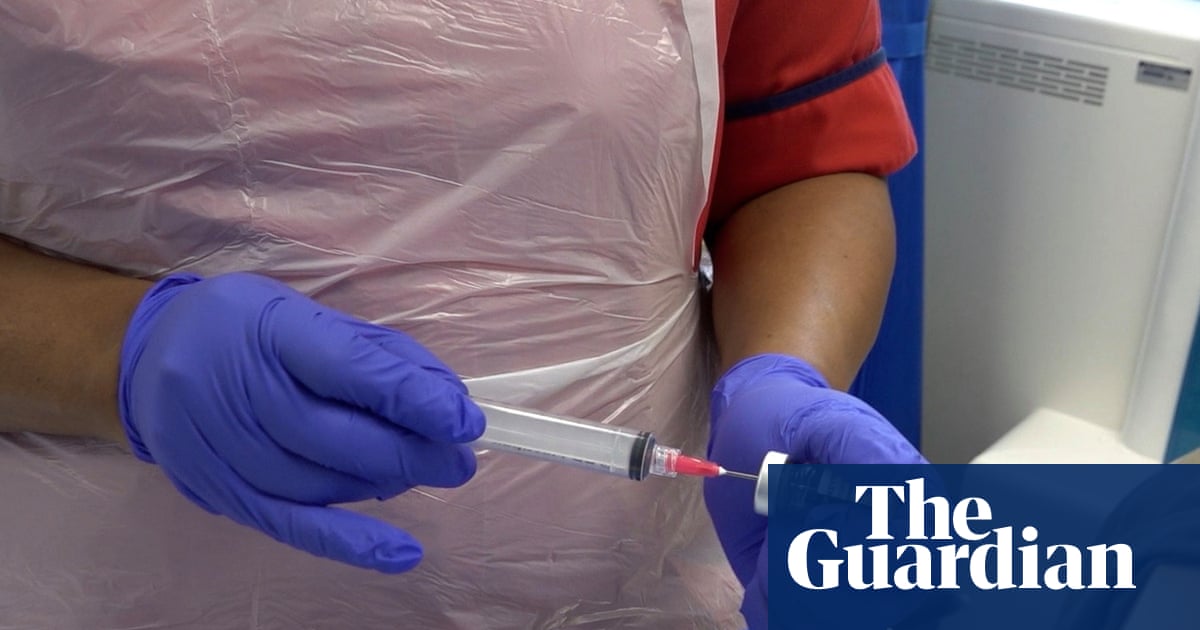
Pembrolizumab blocks the PD‑1 protein, releasing a brake on the immune system so it can attack cancer cells. The drug is approved for nearly 30 cancer types and has been given via intravenous drip in a specialist clean room, a process that takes about two hours per session. The new formulation delivers the same dose as a subcutaneous injection that can be completed in one to two minutes.
Key Facts
- NHS modelling estimates the switch will save more than 100,000 hours of preparation and treatment time annually, based on a cohort analysis of the 14,000 patients currently receiving pembrolizumab. - Professor Peter Johnson, NHS national clinical director for cancer, said the rapid jab "offers a lifeline to thousands of patients" and frees them from long hospital stays. - Approximately 14,000 patients already on pembrolizumab are slated to receive the injectable version. - An additional immunotherapy, nivolumab, which requires three to five minutes, is already available; together they expand injectable options for almost 30 tumour types on the NHS.
What It Means
Patients will spend far less time in chairs, allowing them to resume daily activities sooner. Clinical teams gain capacity to treat more people, potentially reducing waiting times. The time saved is a direct causal effect of changing the delivery method, assuming treatment frequency stays at every three or six weeks. Practical takeaway: faster administration can improve both patient experience and staff efficiency without altering drug efficacy.
What to watch next: real‑world uptake rates and any impact on treatment outcomes or NHS cost‑effectiveness over the coming year.
Continue reading
More in this thread
Three Dead, Three Ill on Atlantic Cruise Ship in Suspected Hantavirus Outbreak
Dr. Priya Sharma
Kenya’s AI‑driven health scheme overcharges the poor, leaves millions unpaid
Dr. Priya Sharma
Kenya’s AI Health Scheme Overcharges Poor, Undercuts Rich, Sparks Protests
Dr. Priya Sharma
Conversation
Reader notes
Loading comments...